Introduction
Welcome to ‘Conversations’ our new central hub to connect with you and pass on any useful information relating to your HIV care.
Please check back here regularly for updates, useful links, changes to service provision and health & wellbeing advice. We welcome any comments using the feedback options below.
– The Sexual Health Team


Chichester Peer Support Group
Upcoming dates 1-3pm
-
Sat 20 September
-
Sat 18 October
-
Sat 15 November
Welcome to the Chichester Peer Support Group!
Connecting with fellow individuals living with HIV (PLWHIV) can be an incredibly empowering and uplifting experience.
The Sussex Beacon is here to offer a welcoming environment where you can express your thoughts, share your journey, and provide mutual support regarding the challenges and triumphs of living with HIV.
We invite participants to bring up any topics they feel comfortable discussing in this respectful and open forum, regardless of their backgrounds.
If some attendees prefer to listen rather than speak, that is absolutely acceptable too.
An HIV-positive facilitator will always be available to guide and support our conversations.
Join us for some light snacks and engaging discussions about what it means to thrive while living with HIV. We will also explore the various services provided by The Sussex Beacon and how to make the most of them.
Refreshments, including tea, coffee, and snacks, will be available.
Location:
The Community Hall, Donegall Avenue, Roussillon Park,Chichester,PO19 6DF.
For further information, please reach out to Alan at alan.spink@sussexbeacon.org.uk or call 07719987054. Or contact Lucy Lucy.h@sussexbeacon.org.uk
15/10/2025
🌻 Reminder: Saturday 18th Peer Support Group 🌻
Hi everyone,
Just a little reminder that our peer support group is meeting on Saturday 18th 1-3pm. We’ll be gathering in our usual space, and we’d love to see you there.
This is a safe, welcoming place where you don’t have to be anything other than yourself. Whether you feel like sharing, listening, or just being present, you are truly welcome.
We’ll be exploring some gentle ways to support ourselves and each other—and you might leave feeling a little lighter, a little stronger, or simply more connected.
peer support is such a valuable tool to support our mental wellbeing and create connection.
Looking forward to seeing you if you’re able to come 💚
Warmly,
Lucy & Alan
venue, The Community hall, Donegall avenue, Roussillon park, PO19 6DF.
Chichester Peer Support Group
New peer support group dates added!
-
Sat 22 Mar (1-3pm, Chichester Sexual Health),
-
Sat 3 May (venue TBC)
-
Sat 14 Jun (venue TBC)
Welcome to the inaugural Chichester Peer Support Group!
Connecting with fellow individuals living with HIV (PLWHIV) can be an incredibly empowering and uplifting experience.
The Sussex Beacon is here to offer a welcoming environment where you can express your thoughts, share your journey, and provide mutual support regarding the challenges and triumphs of living with HIV.
We invite participants to bring up any topics they feel comfortable discussing in this respectful and open forum, regardless of their backgrounds.
If some attendees prefer to listen rather than speak, that is absolutely acceptable too.
An HIV-positive facilitator will always be available to guide and support our conversations.
Join us for some light snacks and engaging discussions about what it means to thrive while living with HIV. We will also explore the various services provided by The Sussex Beacon (https://www.sussexbeacon.org.uk/) and how to make the most of them.
Refreshments, including tea, coffee, and snacks, will be available.
Location:
St Richard’s Hospital, Sexual Health Centre, PO19 6SE (find us on Google Maps)
For further information, please reach out to Alan at alan.spink@sussexbeacon.org.uk or call 07719987054.

28.02.2025
21.01.2025
Chichester Peer Support Group

Saturday 8th February 2025
13:00 – 15:00
St Richard’s Hospital, Sexual Health Centre, PO19 6SE (find us on Google Maps)
11.12.2024
Message from the Sussex Beacon
New memory and HIV website
We are excited to announce the launch of our co-produced website, designed to provide tailored information about cognitive impairment in people living with HIV.
For patients and caregivers, this resource offers clear explanations of what cognitive impairment is, practical guidance on how to recognise it, and helpful tools to improve brain health and access support.
For healthcare professionals, the website provides valuable resources on identifying and managing cognitive impairment, even in settings where neurocognitive testing may be limited.
Our goal is to empower both individuals and healthcare providers with the knowledge and resources they need to improve care and outcomes for people living with HIV.
Explore the site and find out more!
12.11.2024
NEW DEVELOPMENTS IN HIV TREATMENT
Exciting new ways to treat HIV are in the pipeline!
These include:
- Long-acting injectable treatment that only needs to be taken twice a year
- New drugs that trick HIV into reproducing too early and cause it to self-destruct
- New drugs that force HIV out of hiding so that the immune system can find and destroy it
- Special antibodies that can last for up to six months which stick to the virus and kill it
- Molecular scissors that can identify and cut out the HIV from cells where it is hiding
To find out more about these developments click here
10.11.2024
Terrence Higgins Trust – Support for building work skills & confidence
Closing date for applications of interest: Monday 9 December 2024.

Our next personal development, work and skills programme starting in January 2025 is designed to support you if:
- You’re unemployed and looking to prepare to apply for work, volunteering or further study.
- You’re in unsuitable or unsustainable work or would like to explore a change in job or career.
- You’d like to build confidence through exploring your skills, strengths and opportunities and challenge barriers.
- You manage long term health conditions and would like help to return to work or volunteering.
- You are looking for part time work because of your welfare benefits or are navigating the Home Office immigration system.
We can support you to take positive steps back towards suitable and sustainable personal development goals in a safe, confidential and supportive environment and in a way that suits you.
The three months programme is available to anyone living with HIV in the UK who is looking for a safe peer-supported space to connect with others and learn about applying for work, identifying their skills, setting professional goals and planning how to achieve them. As well as offering guidance, support and an accountable plan of action, bespoke to your needs and ambitions along with a dedicated Work and Skills mentor for the duration of the course. There will also be the opportunity to attend additional workshops on Welfare Benefits and the Equality Act, disclosure and reasonable adjustments in the workplace.
The online sessions are interactive and include a mixture of information, confidence building and small group discussions to share ideas and learning. There will be the option for people based in and around London to attend some in person/hybrid training sessions however the whole online the course if open to anyone anywhere in the UK.
If you’re living anywhere in the UK, you’ll be able to access the programme online through Zoom group webinars, along with online one-to-one mentoring and peer support.
How do I get involved?
We’re now accepting applications of interest for our next intake.
If you’d like to register your interest for the programme or would like to find out more, please complete the short form on our web page. https://www.tht.org.uk/our-services/living-well-hiv/work-and-skills
Our Employment Support Officer will get back to you to arrange a short assessment.
Closing date for applications of interest: Monday 9 December 2024.
If you’re looking for group support with your wellbeing and living with HIV, see our Groups and Workshops page for more information: https://www.tht.org.uk/our-services/living-well-hiv
Latest news and advents:

New HIV support in West Sussex
Lunch Positive is a community based HIV charity that provides a wide range of peer-led support. This includes HIV Lunch Clubs where in dedicated, confidential community spaces people spend relaxed and supportive social time together, sharing an enjoyable meal and peer-support. These also link with help from specialist workers, advice and information, wellbeing activities, food bank and home outreach. Our services are provided by volunteers alongside a Support Worker, and because of the amazing contributions of people living with HIV in volunteering we were recently awarded the Queen’s Award for Voluntary Service.
We are looking to establish new support in West Sussex, focussing on providing regular social, support and peer gatherings around a shared meal, similar to our popular HIV lunch clubs elsewhere. As with all our work, these would be led and provided by and for people living with HIV. We need your help to know what’s needed and how this should work in West Sussex. We’re also looking for people who might want to get involved as volunteers.
Please help by completing the survey, which can be done anonymously if you wish. When we have received everyone’s responses we’ll publish an update on progress. We’ll also get in touch with people who have asked us to. If you have any questions you can contact us at hello@lunchpositive.org or call 07846 464384. Thanks so much for helping.
Link to survey: https://lunchpositive.org/community-support-in-west-sussex-survey-2023/

HIV & Self-Stigma
Peer-led Workshop A group for women living with HIV
Friday 26th May: 10:30am – 3pm
at The Sussex Beacon
Lunch is included
“Internalized stigma” or “self-stigma” happens when a person takes on the negative ideas and stereotypes about people living with HIV and starts to apply these to themselves.
This is our second workshop on self-stigma. This time it will be led by Lucy Hutchinson, who is our Peer Mentor Coodinator and is a woman living with HIV. She will share her own experiences and invite women attending to share their own experiences and advice in a safe and confidential space.

Please do let me know if you wish to attend as we need numbers for lunch so the chef can prepare enough food. Please let me know if you have any allergies or food preferences even if you’ve informed us previously so we can make sure we have food you can enjoy!
You can reply to this email or call/text/Whatsapp me on 07530 425624.
Professionals: please circulate to women who may be interested.
Kind regards,
Eve O’Hanlon
Women & Families Worker
Tel: 01273 694222 ext. 263
Mobile: 07530 425624
Email: evelyn.ohanlon@sussexbeacon.org.uk
Kick-start 2023
2022 was a challenging year for many of us. As we start 2023, it’s time to think about what you can do to improve your health and wellbeing. Not by making resolutions that you break within days, but a more sustainable set of SMART (specific, measurable, achievable, relevant, time-bound) goals that help you achieve positive improvement to your wellbeing.
Our Winter Wellness sessions can help if you’re worried about what 2023 has in store, want to build up your confidence, look for a new job or hobby, get fitter, or improve your diet – especially if you aren’t sure how to motivate yourself to come up with a workable solution.
You can also attend if you just want to chat about anything in confidence with one of our volunteer peer mentors who are living with HIV.
Join us at either or both sessions, and look out for other events to support your winter wellbeing.
All information and details for how to join us for these events can be found at:
Living well with HIV | Terrence Higgins Trust (tht.org.uk)
Winter Wellness Tea and Chat (London, in person)
Date: Wednesday 18 January 2023, 2pm to 4pm.
This option is for people living in or around London who want to join in person at our new Cally Yard head office.
We’re located at 439 Caledonian Road, Islington, N7 9BG. The nearest tube station is five minutes walk at Caledonian Road on the Piccadilly line.
Volunteer Peer Mentors will be available to talk to anyone in confidence.
Light refreshments will be provided.
Email livingwell@tht.org.uk to let us know you wish to attend in person.
Winter Wellness Tea and Chat (Nationwide, online)
Date: Wednesday 25 January 2023, 12pm to 2pm.
This option is for people who live outside London or those who prefer to join remotely via Zoom, from home or elsewhere.
Register for this online event
09.01.2023

A new online training programme, running live with a Q&A session, with episodes then available via the UK-CAB website, begins on Tuesday 10 January 2023, 7pm–8pm. It will run every fortnight and aims to inform people living with HIV about evidence-based medicine, clinical trials and the history of treatment and advocacy.
It starts with an outline of how the AIDS epidemic began, the impact on the general population, and the rise of AIDS activism, followed by a panel discussion from three people who lived through this period. To find out more and register for the course, go to the UKCAB website here.
Membership of UK-CAB is free to anyone living with, affected by HIV, or working in the HIV sector.
16.06.2022
Sussex Beacon
Mindful Living Course For People Living with HIV in Sussex- September 2022
“2 Hours a week for 9 weeks can change your life”
This Mindfulness Course is Open to anyone living with HIV in Sussex.
It will run over 9 weeks, and it will build skills to help with problems linked to stress, including low mood, anxiety and pain. The course offers a practical approach to developing skills and understanding for improving health and well-being, in a safe and inclusive environment.
Once completed you are invited to join our continuing development sessions, held regularly at the Sussex Beacon and on-line. It offers a supportive, safe, mindful community.
Call the Sussex Beacon on 01273 694222 for more information.
29/04/2022

On 21st February 2022 the Joint Committee on Vaccination and Immunisation (JCVI) published advice on spring COVID booster vaccines [1]. The JCVI is the national group that advises the government on vaccines. JCVI recommends offering a “spring vaccine” dose to individuals aged 12 years and over who are immunosuppressed, including all people with HIV, about 6 months after their last vaccine dose.
Based on previous recommendations, most people living with HIV will already have had a 3rd or 4th vaccine dose. This spring dose could therefore be their 4th or 5th dose of vaccine.
Many people with HIV are not thought to have a weakened immune system. For some the risk of becoming very unwell with COVID is similar to that for people without HIV. Offering a spring booster to all people with HIV keeps things simple and ensures that everyone at higher risk is protected.
BHIVA strongly encourages all people living with HIV to have the recommended COVID vaccines. Responses to first and second vaccine doses can be lower in some people with HIV, particularly those with a damaged immune system (a CD4 count less than 350 or with a detectable HIV viral load.) These people are a particular priority for extra vaccine doses which should boost their immune responses.
How to get your vaccine dose
Your HIV clinic will have information on vaccination. You will be able to book online if you are eligible for another dose:
https://www.nhs.uk/conditions/coronavirus-covid-19/coronavirus-vaccination/book-coronavirus-vaccination/
Most people with HIV should have had 3 vaccine doses. People at higher risk (lower CD4, detectable viral load, or other risks for severe COVID) should have had 4. Some of the vaccines have been coded differently, as a third dose OR a booster, but that is not important as long as you get the correct number in total.
Some people with HIV received an extra vaccine dose (i.e. a 4th dose) although they did not need it, as they were not at greater risk. If this is the case, BHIVA recommends that a spring Booster should still be given about 6 months after the most recent dose (i.e. 5 doses total).
People who have not been vaccinated at all
BHIVA strongly recommends that everyone living with HIV should have COVID vaccines to protect them. People who have not yet had the COVID vaccine, but who would now like to, should tell their doctor that this will be their first course of vaccine. BHIVA recommends that the first 2 doses should be 4 weeks apart (or the shortest gap approved for the specific type of vaccine,) followed by extra doses in line with the intervals listed below.
Timings
Based on JCVI advice:
The 3rd vaccine dose, only if required – check with your HIV clinic – should be given at least 8 weeks after the 2nd and as soon after that time point as possible.
Autumn 2021 boosters should be given at least 3 months after the 2nd or 3rd vaccine dose.
Spring 2022 boosters should be given around 6 months after the last vaccine dose.
Vaccine type
JCVI recommends that:
eligible persons aged 18 years and over are offered booster vaccination with 30mcg Pfizer-BioNTech (Comirnaty) vaccine or 50mcgModerna (Spikevax) vaccine.
eligible persons aged between 12 and 18 years are offered booster vaccination with 30 mcg Pfizer-BioNTech (Comirnaty) vaccine.
New vaccine products, including vaccines which are more closely matched to future circulating virus(es), may become licensed and available in 2022.
References
1) https://www.gov.uk/government/publications/joint-committee-on-vaccination-and-immunisation-statement-on-covid-19-vaccinations-in-2022/joint-committee-on-vaccination-and-immunisation-jcvi-statement-on-covid-19-vaccinations-in-2022-21-february-2022#fn:1
2) Greenbook COVID-19 chapter 14a (publishing.service.gov.uk)
3) C1399-Updated-JCVI-guidance-for-vaccinating-immunosuppressed-individuals-with-third-primary-dose.pdf (england.nhs.uk)
For further information, please contact bhiva@bhiva.org or for media enquiries, please contact Jo Josh at jo@commsbiz.com or +44 (0)7306 391875.

@ Sussex Beacon
- Friday 20th May 2022: Guest speakers from the Terrence Higgins Trust including Positive Voices and a Welfare Rights Q&A
- Friday 10th June 2022: Creative wellbeing: Summer flower wreath making
- More details to follow.
![]()

03/02/2022

07/01/2022
Befriending programme available for people living with HIV
Sound interesting?
Taking the first step is easy. Just get in touch!
The scheme is open to anyone living with HIV and is available in Brighton & Hove and across Sussex.
If would like to find out more about how the scheme works, being matched with a volunteer or becoming a volunteer then please get in touch with Lunch Positive using the form below or call us on 07846 464384
More information can be found here:
https://www.lunchpositive.org/befriending/
Living well with HIV – THT
Kickstart the new year workshops (peer learning) Our free and confidential online living well and work and skills group aims to kickstart you into 2022. The sessions will be hosted on Zoom, with the focus on participant discussion and peer sharing.
More information can be found here:
https://www.tht.org.uk/our-services/living-well-hiv
22/12/2021
New treatments for coronavirus
The NHS is using new treatments for coronavirus. Some people living with HIV may benefit from these treatments if a PCR test confirms that you have coronavirus. These treatments can stop you from getting seriously unwell from coronavirus but need to be given quickly after you start to feel unwell.
If your GP has your HIV status recorded, you will have already been identified as someone who might benefit from treatment. You may have already received a letter (C1503_ii_Letter to patients about new COVID-19 treatments_201221) from NHSE and you may be contacted automatically to discuss treatment if you test positive. Only those eligible after assessment will be offered treatment.
If you have been diagnosed in the last year or your GP is not aware of your status you will receive a letter from us confirming that you may fulfil the criteria for treatment.
We recommend that you keep a COVID PCR test at home.
Click this link for more information https://www.bhiva.org/update-on-COVID-treatments-for-people-with-HIV
Living Well Programme 10/12/2021

02/12/2021 – Sussex Beacon News
![]()

19/11/2021
Injectable ARVs
After the news was announced via the media yesterday (18/11/2021) we have already had queries regarding the availability of injectable ARVs (cabotegravir and rilpivirine)
At this early stage we are unable to comment on service availability. Your local HIV team will keep you posted on any developments and we advise you to discuss this with them at your next routine appointment
The recently published NICE guidance can be found here:
https://www.nice.org.uk/guidance/gid-ta10658/documents/html-content-2
In the meantime, please check back here for any service updates.
25/05/2021
Update from the Sussex Beacon
13/04/2021
Update from the Sussex Beacon
Women’s Group Online – Ask an HIV Consultant
WHAT: Online Women’s Group with question and answer session with an HIV Consultant
WHEN: Friday 23rd April – 12:30 – 2pm
WHERE: Zoom
Yvonne Gilleece is an HIV Consultant at the Lawson Unit who specialises in Women’s Health, and we are lucky enough to have her join us for an online session to speak about women and HIV and answer any questions you have. It is a really good opportunity to speak to a clinician directly, particularly as many of us have not seen their consultant for a long time due to covid, so please don’t miss out.
Please note this online group will take place at the different time and day of 12:30 – 2pm Friday 23rd April. I really encourage you to come if you are able, as it is a very important opportunity to speak to Yvonne, and bring any questions you have.
Topic: Women’s Group – HIV Clinician Q&A
Time: Apr 23, 2021 12:30 PM London
Click to Join Zoom Meeting
https://us02web.zoom.us/j/83575336890
Meeting ID: 835 7533 6890
Passcode: Beacon111
Using Zoom:
You can access Zoom for free if you have a smartphone, laptop or tablet (like an ipad or other brand), and you don’t need to sign up for an account to use it. Just click on the above link, or use the sign in details listed above.
Any problems please let me know by emailing me or texting or calling me on the number below.
Lou Thomas
Women and Families Group Coordinator
07530 425624
lucy.thomas@sussexbeacon.org.uk
30/03/2021
Update from the Sussex Beacon
![]()
Dear All
I hope that you are keeping well.
I would like to introduce Eve O’Hanlon. She will be leading the Day Service Group , facilitating and developing the service.
We are very excited to have her on board and I know she would like to meet with you all.
Please bear with us, as she works Tuesday and Wednesdays only, it may take time to get in touch.
In the meantime do feel free to contact myself or Eve directly should you wish.
In general our community services are running as follows:
- Day Service – Tuesdays and Wednesdays – Face to face
- Women’s groups – Face to face and online. Next face to face 9th April.
- Peer mentoring – Face to face and on line – we are adapting to what works best for the clients.
- Mindfulness – on going development sessions face to face and on line . Accepting referrals to go on a waiting list for new courses
- Positive Fitness Class – online and face to face.
- Casework and Community support work- face to face
- Our services are for all people living with HIV across Sussex.We are accepting referrals for all services, including the inpatient unit, through our on line secure form.
We are happy to take phone calls and emails directly too.
With best wishes
Hattie
Hattie Yannaghas
Community Services Manager
Health Management Team
The Sussex Beacon
17/03/2021
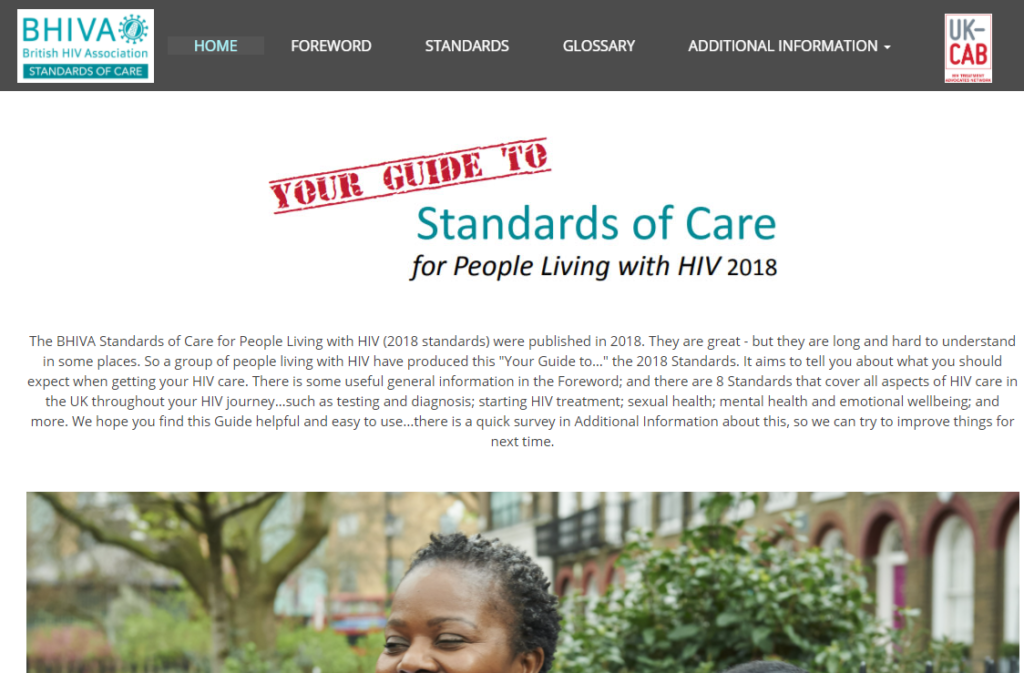
Your Guide to BHIVA Standards of Care for people living with HIV
This guide to the 2018 BHIVA Standards of Care has been specially designed for people living with HIV so that they have the key information in a more user-friendly format about what they can expect when accessing HIV care. The guide follows the full 2018 Standards, covering all aspects of HIV care such as testing and diagnosis, starting HIV treatment, sexual health, mental health and emotional wellbeing.
Click the image below for the full article:

10/03/2021
Update from the THT


12/02/2021
COVID-19 Vaccine for persons living with HIV
Introduction
The UK was the first country to approve the use of a COVID-19 vaccine, which is being referred to as ‘The Pfizer vaccine,’ and vaccination with this started on the 8th December 2020. There is also another vaccine, known as ‘the AstraZeneca vaccine’ or ‘the Oxford vaccine,’ which has also been shown to be very effective at preventing COVID-19 and vaccination with this started on 4th January 2021. Other vaccines are also in the pipeline, including the Moderna vaccine, which was approved for use in the UK on 8th January 2021, with first vaccinations expected in the Spring.
The patient information leaflets for the three currently approved COVID-19 vaccines (Pfizer/BioNTech, AstraZeneca/Oxford and Moderna) all list a weakened immune system under the warnings and precautions for use, with Pfizer using HIV as an example. The leaflets advise affected patients to tell their doctor, nurse or pharmacist before vaccination. The British HIV Association has contacted Pfizer to challenge the mention of HIV in the leaflet.
This advice in the patient information leaflets is not based on concerns about safety. There is currently no evidence for more side effects in people with HIV. The guidance is there mainly because there is not yet very much research information about people with immune deficiency and/or HIV.
With some vaccines, people with HIV can produce a weaker response. We do not yet know if this is the case for the COVID-19 vaccines but they are expected to be protective in people with HIV and are recommended.
Are the vaccines live?
None of the COVID-19 vaccines contain any live virus and so cannot cause COVID-19. The AstraZeneca/Oxford vaccine contains a cold virus, called adenovirus, which has been changed to make it inactive; similar adenovirus vaccines have been used and studied in populations where HIV is common and have been shown to be safe. All currently approved vaccines are thought to be safe for people with suppressed immune systems.
Is there any interplay between COVID-19 vaccine and HIV drugs?
No. HIV drugs do not affect the effectiveness of COVID-19 vaccines and COVID-19 vaccines do not affect how well HIV drugs work either. If you have had side effects or an allergic reaction to particular HIV drugs in the past, that does not mean you will get side effects from the COVID-19 vaccines.
There is no evidence that HIV drugs, taken as HIV treatment or prevention (PrEP) can be used to prevent or treat COVID-19. Some studies are looking into using HIV drugs to prevent COVID-19 but there are no results yet and no good evidence to suggest they will be effective.
Who will be prioritised to get the vaccine early?
People will receive the vaccine in strict order of priority based on their age, health, occupation, whether they live in a care or residential home and who they live with. Vaccines will be offered strictly based on these priorities. There is no way to jump the queue, and you will be contacted when your vaccine is due.
There are 9 priority groups: those in priority group 1 will get the vaccine first, followed by each in turn up until priority 9. After that the vaccine will be offered to everyone else (that is all the people not in priority groups 1-9).
Will persons living with HIV be prioritised for the vaccine?
Everyone living with HIV fall into the Priority group 6: people with underlying health conditions which put them at higher risk of serious disease and mortality.
A small proportion of people living with HIV will fall into Priority group 4 (Clinically Extremely Vulnerable).
This includes individuals with a CD4 count less than 50 cells/mm3, or who have had an opportunistic illness in the last 6 months. Individuals with a CD4 count in the range 50-200 cells/mm3, with additional risk factors may also be added to this category following assessment by their clinician.
In West Sussex we have reviewed all patients accessing care through our service and have identified and contacted ALL individuals who fall into priority group 4. If you have not been contacted by the Consultant responsible for your care, you do not fall into this category in relation to your HIV status (you may of course have been contacted by your GP and placed in this category for non-HIV related reasons).
If you have not already received a COVID vaccination for other reasons, you will be eligible for vaccination in priority group 6. The national vaccination programme will shortly be moving onto this group and therefore you will receive a text message from the West Sussex HIV service in the next couple of weeks, confirming your eligibility for priority vaccination and advice to contact your GP.
Who do I contact if I have questions?
There are a lot of false rumours circulating about the COVID vaccines which has created concern and low vaccine uptake, particularly in some with higher risk of severe disease or death from COVID infection.
The British HIV Association (BHIVA) www.bhiva.org has lots of information about COVID, vaccination and HIV.
If after reading the information available you have questions about the safety or effectiveness of the vaccine, please contact your local clinic to discuss your concerns with your Doctor.
If you want to receive the vaccine please contact your GP for advice on local vaccination centres. We are unable to offer you the vaccine in your HIV clinic. You can use the text received from our service as evidence for your eligibility in priority group 6.